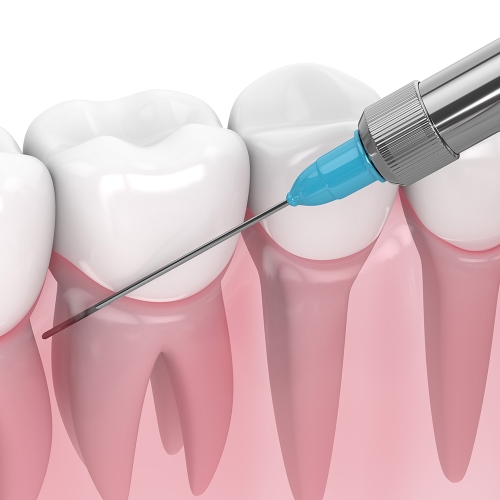
Injectable Anaesthetics for Pain Control During Dental Procedures
Anaesthetics are used during dental procedures to make patients comfortable and, in some cases, restrict bleeding in the surgical area (e.g. Artinibsa 4% 1:100,000 solution for injection). However, special considerations need to be made for patients with pre-existing renal and hepatic impairment. Additionally, providers who use local anaesthetics should closely monitor patients with these pre-existing conditions and be aware of signs of toxicity.
Anaesthesia and Renal and Hepatic Impairment
Local anaesthetics are metabolised by the liver through a biotransformation into water-soluble metabolites. Specifically, microsomal enzymes found in the liver perform this transformation — once metabolised, it is then excreted through the urine.
In patients with renal and hepatic impairment, the ability to both breakdown and excrete the metabolites becomes inefficient. This can lead to the accumulation of metabolites in the blood, which can be further compounded by repeat dosing of the local anaesthetic. With this, understanding how different anaesthetics are metabolised can help determine which to use and the dosing.
Artinibsa Solution for Injection
Artinibsa is made using 40 milligrammes (mg) of articaine with 5 or 10 microgrammes (µg) of adrenaline. Much of the molecule is inactivated by enzymes (known as plasma esterases) found in the tissues and blood. However, patients with hepatic impairment should be given the lowest dose possible to prevent adverse effects or toxicity. Patients with renal disorders should also be monitored, especially when being given repeat doses.
Xilonibsa Solution for Injection and Spray
Xilonibsa is administered by one of two ways — as a pulsing dispenser containing 10 mg of lidocaine spray, or 20 mg lidocaine with 0.0125 mg of epinephrine as an injection.
Lidocaine is metabolised by the liver, so patients with underlying hepatic impairment will have a difficult time processing the molecule. The half-life of lidocaine may be extended by two-fold or more in patients who have hepatic impairment. With this, the dose is lowered to allow time for the anaesthetic to be cleared from the body.
Patients with nephritic syndrome should receive a reduced dose in order to prevent accumulation of metabolites in the blood. These patients have a low capacity of plasma proteins to bind lidocaine and its metabolites.
Scandinibsa Solution for Injection
Scandinibsa is an injectable solution that contains 30 mg of mepivacaine hydrochloride. It is primarily metabolised by the liver, specifically by microsomal enzymes such as cytochrome P450 1A2.
Over 50% of the dose is then excreted into the bile as metabolites. With this, patients with underlying liver hepatic impairment should receive a lower dose of mepivacaine. Lower doses of mepivacaine should also be used in patients with renal impairment; closely monitor patients who need repeat dosing.
Inibsacain Solution for Injection
Inibsacain is an injectable solution that contains 5 mg of bupivacaine and 0.005 mg of epinephrine. Patients with advanced hepatic impairment/disease and severe renal dysfunction should be monitored closely when given bupivacaine.
According to the U.S. National Kidney Foundation, 10% of the world’s population is affected by chronic kidney disease. Liver disease is also thought to affect between 4.5% to 9.5% of the general population. With this, dentists can expect to treat more patients with these underlying health conditions, highlighting the need for understanding how local anaesthetics affect this population.
References
- Malamed, S.F. Handbook of Local Anesthesia. 7th. ed.- St. Louis, MI : Elsevier Mosby, 2020.
- Daskalov H. et al. Local anesthetics in patients with cardiovascular diseases. J of IMAB. 2015;21(1):728-731.
- Moore P.A. et al. Hemostatic and anesthetic efficacy of 4% articaine HCl with 1:200,000 epinephrine and 4% articaine HCl with 1:100,000 epinephrine when administered intraorally for periodontal surgery. J Periodontol. 2007;78(2):247-53.
- Summary of Product Characteristics of Artinibsa 4% 1:100,000, Artinibsa 4% 1:200,000, Xilonibsa 2% 1:80,000, Xilonibsa Spray 10%, Scandinibsa 3% and Inibsacain 5 mg/ml + 0.005 mg/ml.
- Decloux D., Ouanounou A. Local Anaesthesia in Dentistry: A Review. Int Dent J. 2021;71(2):87-95.
- National Kidney Foundation. Global Facts: About Kidney Disease. Retrieved from https://www.kidney.org/kidneydisease/global-facts-about-kidney-disease
- World Gastroenterology Organisation. Global Burden of Liver Disease. Retrieved from https://www.worldgastroenterology.org/publications/e-wgn/e-wgn-expert-point-of-view-articles-collection/global-burden-of-liver-disease-a-true-burden-on-health-sciences-and-economies