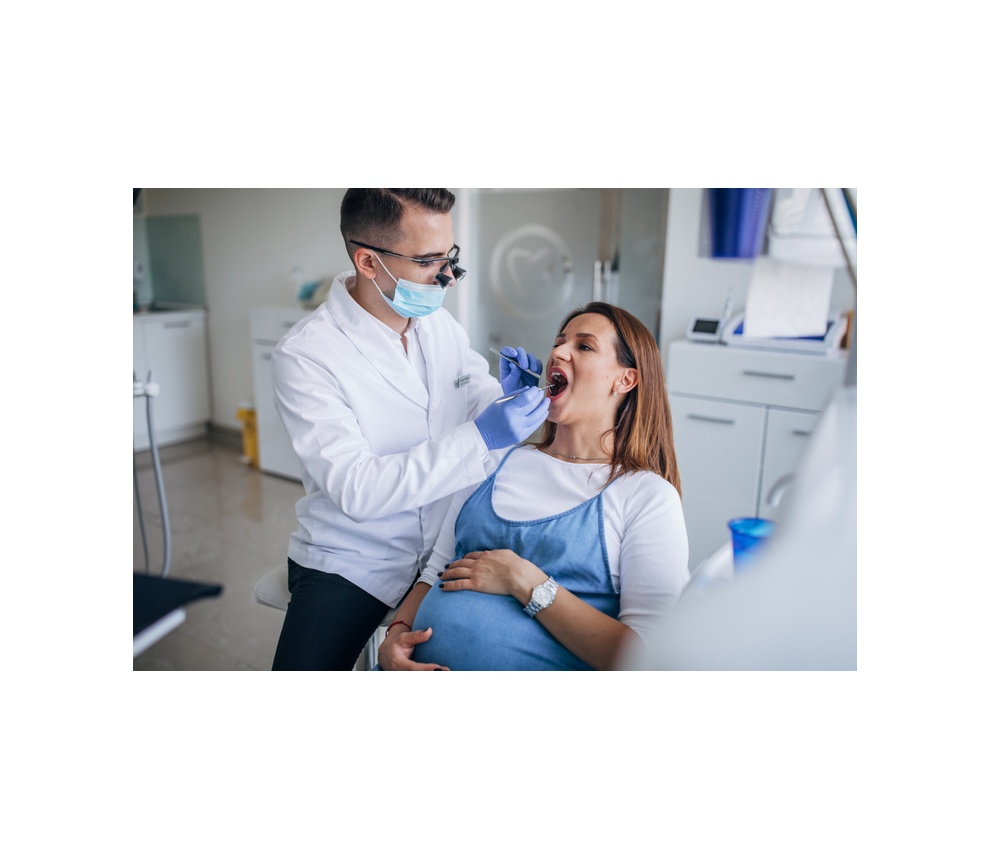
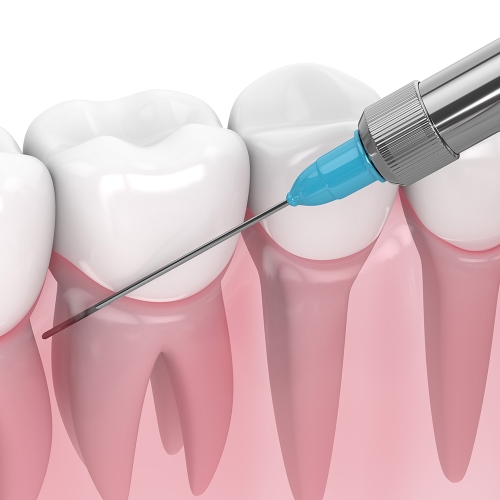
Injectable Anaesthetics for Pain Control During Dental Procedures
Anaesthetics are used during dental procedures to make patients comfortable and, in some cases, restrict bleeding in the surgical area. However, special considerations need to be made for patients who are pregnant or breastfeeding. Additionally, providers who use local anaesthetics should closely monitor these patients to avoid toxicity or any adverse events.
Anaesthesia and Pregnancy and Breastfeeding
Special considerations must be taken when treating pregnant and nursing mothers. Dr. Stanley F. Malamed, DDS, has recommendations for dental care and elective procedures for pregnant women depending on the trimester.
Many pregnant and nursing mothers may express concern for the anaesthetics entering the foetus/newborn. Medications given to pregnant women will travel through the bloodstream to the foetus, but they are not known to have any serious adverse effects. Medications may also be excreted into breast milk in nursing mothers, but these are also not known to have any serious effects.
Elective dental care should be avoided at all costs during the first trimester due to the high risk of spontaneous abortion and foetal malformation — this recommendation is given regardless of local anaesthetic use. The second trimester is believed to be the safest time to have elective dental work. In the third trimester, there is an increased risk of aortocaval compression and increased conduction blockade.
There are no contraindications of local anaesthetic use during pregnancy, but it is best to postpone non-urgent procedures until after the mother gives birth. Local anaesthetics will also be found in breast milk, but there are no contraindications for them with or without epinephrine in nursing mothers. If a local anaesthetic is needed, articaine is best because it has a shorter half-life — the molecule will be eliminated from the body more quickly than other anaesthetics.
The doses of both local anaesthetics with and without epinephrine should be administered at the lowest effective concentration of epinephrine (1:200,000) in order to avoid adverse effects.
Artinibsa Solution for Injection
Artinibsa is made using 40 milligrammes (mg) of articaine with 5 or 10 microgrammes (µg) of adrenaline. Currently, there is little data available on using articaine in pregnant women. It is known that both articaine and epinephrine cross the placental barrier, but less so than the extent of other local anaesthetics.
Articaine is not found in breast milk because it is metabolised and eliminated quickly from the body. Epinephrine can pass into breast milk but it has a short half-life and does not pose a significant risk to the baby. However, it is not usually necessary to stop breastfeeding after using Artinibsa.
Artinibsa should only be used after a careful analysis of the benefit-to-risk ratio, taking into account the health of both the mother and foetus/infant.
Xilonibsa Solution for Injection and Spray
Xilonibsa is administered by one of two ways — as a pulsing dispenser containing 10 mg of lidocaine spray, or 20 mg lidocaine with 0.0125 mg of epinephrine as an injection.
While there are no formalised studies on the effects of lidocaine use in pregnant women, lidocaine is classified as a category B medication by the U.S. Food and Drug Administration (FDA). It is not recommended for use as the molecule can cross the placental barrier. It does not appear to cause harm to the foetus, but it should be reserved for use in cases where the benefits outweigh the risks.
It is also known that lidocaine is excreted in breast milk, but at very low concentrations that should not affect newborns/infants who are breastfed.
Scandinibsa Solution for Injection
Scandinibsa is an injectable solution that contains 30 mg of mepivacaine hydrochloride. There are currently no studies available for use in pregnant women, so it is best to avoid use unless medically necessary. However, animal studies show no direct or indirect harmful effects.
There are also no studies available on the use of mepivacaine in nursing mothers, so the risk of harm to newborns/infants who are breastfed cannot be excluded. With this, nursing is not recommended within 10 hours of receiving mepivacaine injection.
Inibsacain Solution for Injection
Inibsacain is an injectable solution that contains 5 mg of bupivacaine and 0.005 mg of epinephrine. It should only be given during early pregnancy when the benefits outweigh the risks. There is also little information on bupivacaine excretion into breast milk, so it should be used with caution in nursing mothers.
Local dental anaesthetics, when used sparingly in appropriate situations, are safe and effective in pregnant and breastfeeding women. Weighing the benefits and risks, along with choosing the correct local anaesthetic, is the most important role of the dentist when it comes to treating this patient population.
References
- Malamed, S.F. Handbook of Local Anesthesia. 7th. ed.- St. Louis, MI : Elsevier Mosby, 2020.
- Decloux D., Ouanounou A. Local Anaesthesia in Dentistry: A Review. Int Dent J. 2021;71(2):87-95.
- Lee J.M., Shin T.J. Use of local anesthetics for dental treatment during pregnancy; safety for parturient. J Dent Anesth Pain Med. 2017;17(2):81-90.
- Summary of Product Characteristics of Artinibsa 4% 1:100,000, Artinibsa 4% 1:200,000, Xilonibsa 2% 1:80,000, Xilonibsa Spray 10%, Scandinibsa 3% and Inibsacain 5 mg/ml + 0.005 mg/ml.